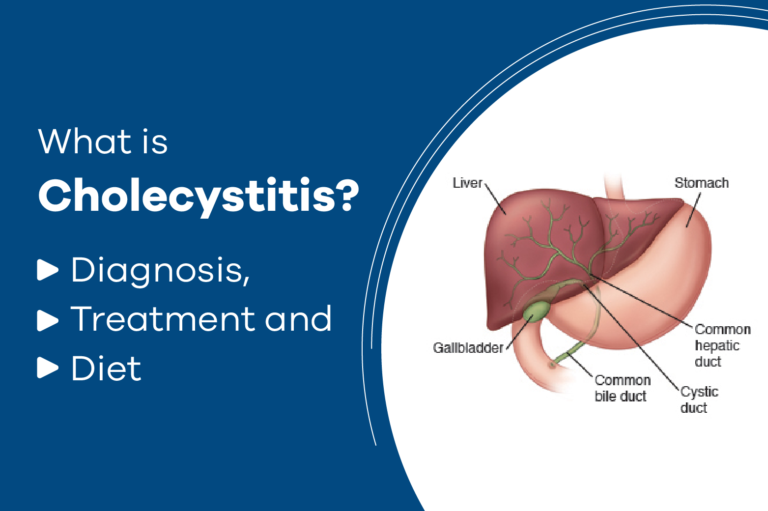
Cholecystitis is an inflammation of the gall bladder. The gall bladder is the small sac-like organ located in the upper right side of the abdomen, just below the liver. It is attached to the main duct that carries bile from the liver into the intestine. The gall bladder temporarily stores bile, which is a liquid that contains a fat-digesting substance produced in the liver. During a meal, bile moves from the gall bladder through small, tube-like passages into the small intestine. Here, bile mixes with food to help break down fats. Cholecystitis usually develops when a person has gall stones, which are rock-like deposits that form inside the gall bladder. Bile gets trapped in the gall bladder. Chemicals in the trapped bile or bacterial infection can lead to inflammation of the gall bladder.
There are two types of cholecystitis
Acute cholecystitis –it is a sudden inflammation of the gall bladder that causes marked abdominal pain, often with nausea, vomiting, and fever.
Chronic cholecystitis – it is lower intensity inflammation of the gall bladder that lasts a long time. It may be caused by repeat attacks of acute cholecystitis. Chronic cholecystitis may cause intermittent mild abdominal pain or no symptoms at all.
Damage to the walls of the gall bladder leads to thickened, scarred gall bladder. Ultimately, the gall bladder can shrink and lose its ability to store and release bile. Gall stones alone can cause episodes of crampy abdominal pain without any infection, known as biliary colic. Women are more likely than men to get gall stones. The risk of gall stones also is higher in the above 60 age group, pregnant women, obese people, women who take oestrogen replacement therapy, birth control pills, due to rapid weight loss, and consumption of high-fat food.
Epidemiology
Cholelithiasis is nothing but gall stones which are prevalent as high as 60 to 70 percent in American Indians and 10 to 15 percent in adults in developed countries. Ethnic differences abound with a reduced frequency in black Americans and those from East Asia as it is rare in sub-Saharan Africa. Certain risk factors for gall stones are immutable, occurring more in females, and may be caused by increasing age and ethnicity/genetic factors. Other factors are modifiable: obesity, metabolic syndrome, rapid weight loss, and certain diseases such as cirrhosis, Crohn’s disease, gall bladder stasis from the spinal cord injury, or drugs like somatostatin or due to lifestyle.
Aetiology
- Severe upper abdominal pain, just below the breast bone or in the upper right portion of the abdomen, near the gall bladder and liver. In some people, the pain extends to the right shoulder, with symptoms typically starting after eating.
- Fever and possibly chills.
- Nausea/vomiting.
- Dark urine and pale, greyish bowel movements.
- These symptoms appear when gall stones pass out of the gall bladder into the common bile duct, blocking the flow of the bile out of the liver.
- When gall stones in the common bile duct block the flow of the bile from the liver to the intestine, the patient may develop a serious infection of the bile ducts called cholangitis.
- The typical symptoms of cholangitis are fever, right upper abdominal pain, and jaundice.
- Another possible problem that may occur when gall stones pass into the common bile duct is acute pancreatitis because the duct from the pancreas also flows into the common bile duct, stones there can block the pancreas, which causes it to become inflamed like cholangitis or acute pancreatitis and become serious.
- The major symptom of chronic cholecystitis is usually intermittent pain. However, some people do not have any symptoms. It may manifest as pain during a sudden attack.
Diagnosis
A physical examination will reveal how tender the gall bladder is. A doctor usually will ask if a patient had any previous history of cholecystitis because it often recurs.
There are certain tests to be ordered
- Ultrasound – This test can highlight any gall stones and may show the condition of gall stones.
- Blood test -This test relieves a high amount of white blood cells that may indicate an infection. High levels of bilirubin, alkaline phosphate, and serum aminotransferase may also help rule out the disease.
- Computerized tomography (CT) or ultrasound scans; images of the gall bladder may reveal signs of cholecystitis.
- Hepatobiliary iminodiacetic acid (HIDA) scan is also known as cholescintigraphy, hepatobiliary scintigraphy, or hepatobiliary scan. This scan creates pictures of the liver, gall bladder, biliary tract, and small intestine.
Untreated acute cholecystitis can lead to
A fistula – a kind of tube or channel that can develop if a large stone erodes the wall of the gall bladder. This can link the gall bladder and duodenum, and the stone may pass through gall bladder distension. If the gall bladder is inflamed because of bile accumulation, it may lead to stretch and swell, causing pain. There is then a much greater risk of perforation, or tear, in the gall bladder as well as infection and tissue death.
Tissue death – gall bladder tissue can die, and gangrene may develop, leading to perforation, or the bursting of the bladder. Without treatment, 10% of patients with acute cholecystitis will experience localized perforation. One percent of patients with acute cholecystitis will experience localized perforation and peritonitis if a gallstone becomes impacted in the cystic duct, leading to cholestasis. This is rare.
Gall stones can sometimes pass from the gall bladder into the biliary tract, leading to an obstruction of the pancreatic duct. This may cause pancreatitis. In 3 to 19 percent of cases, acute cholecystitis can lead to a pericholecystic abscess.
Cholecystitis treatment
Patients who are diagnosed with cholecystitis will have to be hospitalized, and they will probably not be allowed to consume any solid or liquid foods for some time. They will be treated with intravenous liquids while fasting. Medications such as painkillers and antibiotics can be given.
Surgery is recommended for acute cholecystitis because there is a high rate of recurrence from inflammation related to gall stones. However, if there is a low risk of complications, surgery can be performed as an outpatient procedure. If there are any complications, such as gangrene or perforation of the gall bladder, the patient will need immediate surgery to remove the bladder. If the patient has an infection, a tube may be inserted through the skin into the gall bladder to remove the gall bladder, or cholecystectomy can be performed by abdominal excision or laparoscopically.
Laparoscopic cholecystectomy involves several small incisions in the skin. A camera is inserted into one incision to help the surgeon see inside the abdomen and he can be provided tools for removing the gall bladder inserted through other incisions.
The benefit of laparoscopy is that the incisions are small, so patients usually have less pain after the procedure. After surgically removing the gall bladder, the bile will flow directly into the small intestine from the liver. This does not normally affect the patient’s overall health and digestive system. Some patients may have more frequent episodes of diarrhoea.
Diet & lifestyle modification for the prevention
Upon recovery from the condition, it is important to make dietary adjustments that help bring bile production back to normal.
Be sure to eat smaller meals more frequently and avoid large serving or portions as these can upset the system and produce a gall bladder or bile duct spasm.
Avoid high fat and fried foods, including whole milk products, and stick to lean proteins.
Stick to regular breakfast, lunch, and dinner times and do not skip meals. Exercise 5 days a week for at least 30 mins each day. Lose weight because obesity increases the risk of gall stones. Avoid rapid weight loss as this increases the risk of developing gall stones.
If you think you need any medical aid or assistance, reach out to us at Vitality’s Laser Piles Clinic to consult us. We will help you schedule an appointment today, Call us: 910 850 3674.